“Wearable soft mask will be useful for new, cutting-edge sleep and psycho-social studies
From the team that invented physiology-sensing pajamas at the University of Massachusetts Amherst, now comes a new, lightweight eye mask that can unobtrusively capture pulse, eye movement and sleep signals, for example, when worn in an everyday environment.
Senior authors writing this week in the journal Matter are materials chemist and Wearable Electronics Lab director Trisha L. Andrew, with computer scientist Deepak Ganesan and others. They point out that “being able to track pulse and eye movement in a single wearable device will enable a host of sleep and psycho-social studies, in addition to improving the accuracy and usability of gaming and virtual reality headsets.” First author S. Zohreh Homayounfar, will present the findings this week at the online Fall Meeting of the American Chemical Society.
Recording health and behavior signals on or near the face is challenging, notes Andrew, “because most people are really sensitive and reactive to objects placed on their face or head.” Ganesan adds that “up to now, integrating many different sensing elements in one garment seemed burdensome, especially when it comes to small eye masks.”
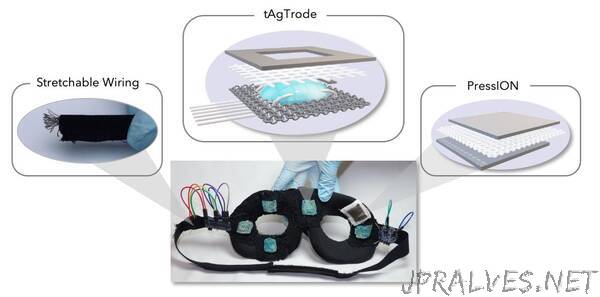
They say their lightweight, tailorable eye mask named “Chesma,” is fitted with two kinds of fabric electrodes that can simply be sewn onto a variety of pre-made garments and further miniaturized, if desired. This capability allows them to integrate electrodes into a lightweight foam mask for recording electro-oculography and cardiac signals. Their design automatically positions the electrodes on the face with no need for custom fitting.
As explained in a video created by Ph.D. student and first author, S. Zohreh Homayounfar, the mask contains five silver (Ag) thread-based hydrogel electrodes –dubbed tAgTrodes – needed to translate ion-based biological signals into an electric current, among other goals. The researchers took advantage of a vapor-phase deposition process to create the electrodes, including what they call a first-of-its-kind reusable and washable hydrogel component that distinguishes the tAgTrode from other equivalents.
Here, Andrew says she takes pride in noting that “part of the work that went into carrying out the deposition process was performed by Emerson T. Alexander, an exceptional student from Springfield Technical Community College,” who took part in a paid internship in her lab and funded by the L’Oréal USA For Women in Science program.
The mask also contains one fabric pressure sensor (PressION) positioned over an artery to monitor pulse as a proxy for cardiac function, with the whole linked to two microcontrollers with water-repellant silver threads as connectors. Another author, Ph.D. student Ali Kiaghadi, explains that “the electrode and sensor data need to be communicated once they are acquired. Our design transmits raw data to the cloud for processing and data visualization, so that we can reduce the amount of instrumentation that we need to include in the mask itself.”
The team tested the new eye mask on subjects while they were chewing, talking, and during various head and eye movements. They also used the same device for more than a year and after 15 washings found no degradation in performance. Homayounfar notes that the tAgTrode “overcomes all the drawbacks of commercial wet electrodes such as aesthetic issues, discomfort and wash-stability, while maintaining high and constant signal-to-noise ratios during repeated, longterm applications.”
Andrew expects that Chesma’s “unique bimodality” – the combination of electrode network with the pressure sensor – will enable many new cutting-edge studies not possible until now, for investigating sleep quality, sleep disorders, mental health, neurodegenerative diseases and schizophrenia, for example.
The work was supported by the National Science Foundation and the David and Lucile Packard Foundation. It was aided by Ganesan and Andrew’s affiliation with the Center for Personalized Health Monitoring at UMass Amherst’s Institute of Applied Life Sciences. where life science research is translated into products to improve human health.”
